How To Get Rid Of Female Visceral Fat
How to Get Rid of Female Visceral Fat (What Actually Works in 2026)
Key Takeaways
- Visceral fat is hormonal, not just dietary. That drop in estrogen during perimenopause? It actively redirects fat storage to your abdomen. Which is why the same habits that kept you lean at 35 stop working at 45.
- The scale lies. Visceral fat loss shows up first in your waist measurement, blood sugar, and energy levels — not your weight. Track the right things.
- One genuinely good thing: this is the most reversible fat you carry. Unlike subcutaneous fat, visceral fat responds quickly to targeted change. Most women see measurable improvement in 6–12 weeks.

You haven’t changed your diet. You haven’t stopped exercising. But somewhere between 42 and 48, your body quietly rewrote the rules — and your waist paid the price.
That firm, swollen belly that won’t budge no matter how many salads you eat? That’s not laziness. That’s visceral fat — and it plays by a completely different set of rules than the soft, pinchable fat on your lower abdomen, subcutaneous fat.
Worse? Visceral fat is largely invisible on the scale. You can be a “healthy” weight by every standard metric and still carry dangerous levels of deep abdominal fat.
This guide covers what visceral fat actually is, how to know if you have it in dangerous amounts, and — most importantly — what research says actually works to get rid of it.
What Is Visceral Fat, and Why Do Women Get More of It With Age?
Location: Visceral fat, a type of belly fat, is the metabolically active fat stored inside the abdominal cavity, packed around your internal organs. You can’t grab it. That’s how you know it’s different.
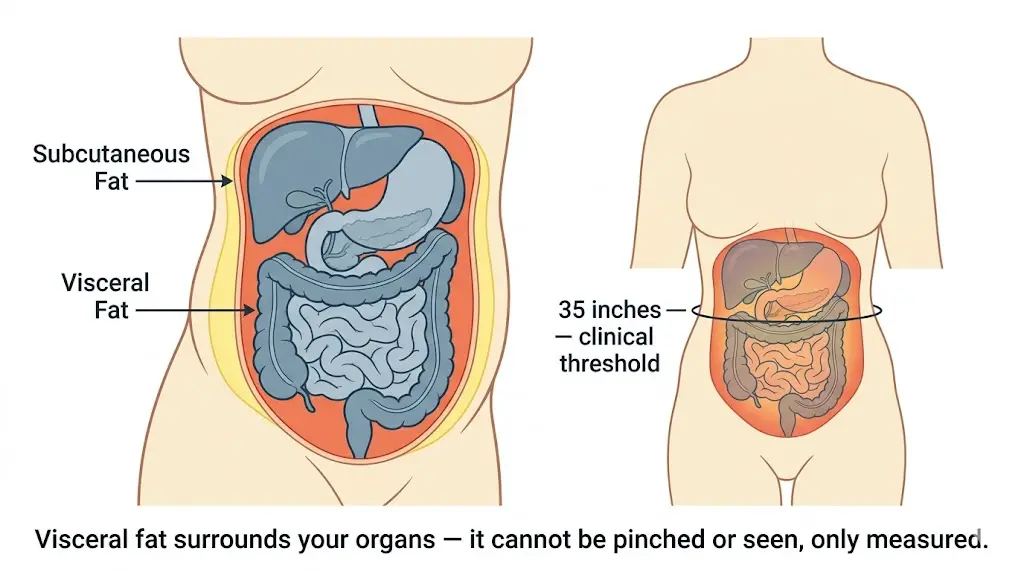
Why is visceral fat dangerous? Visceral fat isn’t passive tissue. It behaves more like an endocrine organ — constantly secreting inflammatory compounds, cytokines, and free fatty acids directly into the portal bloodstream feeding your liver. This is why high visceral fat is independently linked to type 2 diabetes, cardiovascular disease, high blood pressure, and certain cancers — even in women who are not technically overweight.
Why women accumulate it faster after 40: For most of your reproductive years, estrogen acts as a metabolic bodyguard — directing fat storage toward your hips, thighs, and buttocks (subcutaneous depots) rather than the abdomen. As estrogen drops during perimenopause (typically beginning between ages 40–52), this protective routing breaks down. The body defaults to a more similar to a more “male” pattern: central, visceral accumulation.
Here’s the kicker. Research published in Obesity confirms that the menopausal transition is associated with a significant increase in visceral adipose tissue independent of total body fat change — meaning you can gain visceral fat even when your overall weight doesn’t budge.
Then add cortisol. Chronic stress — a fixture of your 40s if you are balancing careers, caregiving, and hormonal upheaval — elevates cortisol levels, which actively drives fat into visceral depots.
How to Get Rid of Female Visceral Fat: What the Research Actually Says
There is no single magic intervention. What works is a protocol — and the research is surprisingly clear about which matters most.
Fix the Hormonal Trigger First: Manage Cortisol and Insulin
Before you change a single meal, understand this: if your cortisol is chronically elevated, your body will resist visceral fat loss regardless of caloric deficit. Cortisol activates glucocorticoid receptors that are particularly dense in visceral adipose tissue — essentially telling your body to keep storing fat there.
Practical cortisol management that has clinical backing:
- Mindfulness-based stress reduction (MBSR): A randomized controlled trial found that MBSR reduced cortisol and visceral fat in overweight women independently of diet changes.
- Prioritizing sleep: Both under-sleeping (<6 hours) and over-sleeping (>9 hours) are independently associated with increased visceral fat. The target is 7–8 hours of quality sleep per night.
The Diet Protocol That Targets Visceral Fat
Increase dietary fiber to 30–40g/day.

Eliminate sugar-sweetened beverages entirely. Fructose — particularly from liquid sources — is metabolized almost exclusively in the liver and is preferentially converted to visceral fat. This is not a “reduce” situation; it’s a hard stop. Sodas, fruit juices, sweetened coffees, and alcohol are the top contributors.
Prioritize protein at 1.2–1.6g per kg of body weight. Higher protein intake increases satiety, preserves lean mass during caloric deficit, and has a higher thermic effect than fat or carbohydrates. For a 150 lb (68 kg) woman, that’s roughly 82–109g of protein daily. This is particularly important post-40, when muscle loss accelerates and preserving lean mass becomes metabolically critical.
Add carotenoid-rich vegetables. Carrots, spinach, kale, red bell peppers, and sweet potatoes are high in carotenoids — pigment compounds with demonstrated anti-inflammatory and anti-adipogenic effects. Studies show higher serum carotenoid levels are inversely associated with visceral fat accumulation.
Consider time-restricted eating (TRE). Compressing your eating window to 8–10 hours (e.g., 10am–6pm) without caloric restriction has shown reductions in visceral fat in clinical trials. The mechanism appears to involve improved insulin sensitivity and alignment with circadian rhythm. This is different from aggressive fasting and is generally well-tolerated by perimenopausal women.
Exercise: The Two Non-Negotiables
HIIT (High-Intensity Interval Training) HIIT is the most time-efficient exercise modality for visceral fat reduction. A meta-analysis of 39 studies found HIIT significantly reduced visceral fat in adults — more effectively than continuous moderate-intensity exercise per unit of time invested. A basic protocol: 20–30 minutes, 3x/week, alternating 30–40 seconds of maximum effort with 60–90 seconds of recovery.
Resistance Training Muscle tissue is metabolically expensive — the more you have, the higher your resting metabolic rate. Resistance training 2–3x/week is the best long-term investment for visceral fat control, particularly post-menopause when muscle loss accelerates. Compound movements (squats, deadlifts, rows, presses) recruit the most total muscle mass and produce the greatest metabolic effect. Follow Rebecca and thank me later.
Note on “spot reduction”: Crunches and planks do not selectively burn visceral fat. Abdominal exercises strengthen the underlying musculature, but visceral fat reduction requires systemic fat loss through the strategies above.
Targeted Add-Ons With Emerging Evidence
Probiotics and gut microbiome support The gut-liver axis is a direct pathway between visceral fat and inflammation. Certain probiotic strains — particularly Lactobacillus gasseri — have shown reductions in visceral fat area in Japanese clinical trials. The Cleveland Clinic notes that probiotics/prebiotics may aid in reducing visceral fat by up to 35%, though larger trials are needed.
Turmeric (curcumin) Curcumin inhibits NF-κB, a master regulator of the inflammatory cascade that visceral fat drives. While it won’t independently reduce fat mass, it directly targets the inflammatory output of visceral adipose tissue. Bioavailability requires pairing with piperine (black pepper).
Capsaicin (chili peppers) Capsaicinoids have thermogenic properties and have shown modest but consistent effects on visceral fat in systematic reviews. Daily intake equivalent to 2–4mg capsaicin — achievable through cooking with chili peppers — is sufficient.
Visceral Fat Female Range: How Much Is Too Much?
There is no universal blood test for visceral fat, but several accessible markers give you a strong signal:
Waist circumference is the simplest and most validated tool. A waist measurement of 35 inches (88 cm) or more in women is the clinical threshold for elevated visceral fat risk, associated with metabolic syndrome and cardiovascular disease.
Waist-to-hip ratio (WHR) adds more context. A WHR above 0.85 in women indicates abdominal obesity and increased visceral fat. Measure your waist at the narrowest point and your hips at the widest, then divide.
Body fat scanner ratings (Tanita/InBody scales) assign visceral fat levels on a 1–59 scale. A visceral fat level of 1–9 is considered healthy, 10–14 is high, and 15+ is very high. These scales use bioelectrical impedance and aren’t perfectly accurate, but they’re a useful tracking tool.
DEXA scan remains the gold standard for quantifying visceral fat precisely. If you have metabolic concerns, it’s worth requesting or paying out-of-pocket for one assessment baseline.

Signs You Are Losing Visceral Fat (Before the Scale Moves)
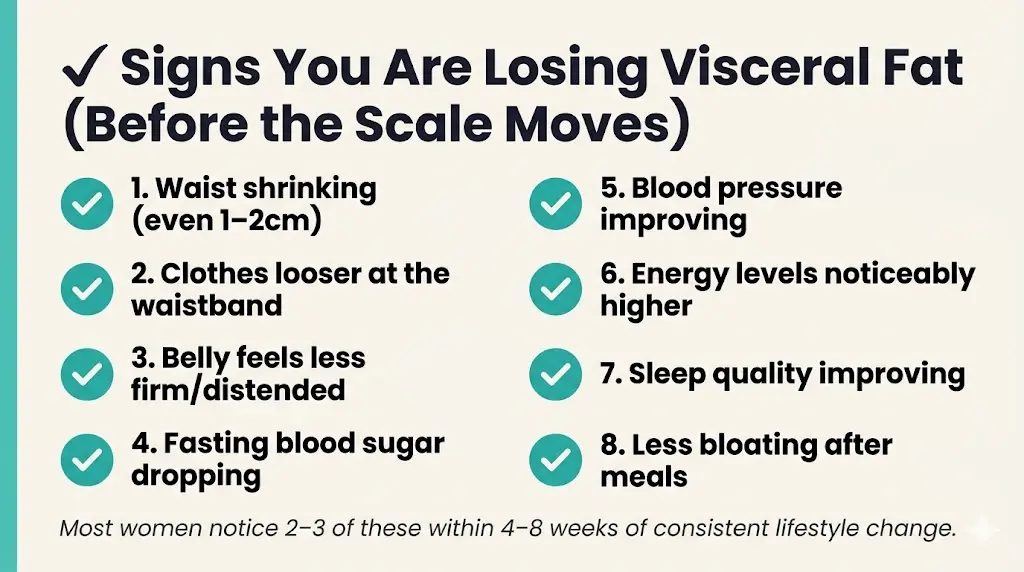
Visceral Fat Symptoms: When Your Body Is Telling You Something
Visceral fat often produces symptoms that get misattributed to stress, aging, or perimenopause:
- Persistent abdominal bloating that doesn’t resolve with digestion
- A firm, distended belly (distinct from soft subcutaneous fat)
- Elevated fasting blood sugar (pre-diabetic range: 100–125 mg/dL)
- Elevated triglycerides (above 150 mg/dL)
- Low HDL cholesterol (below 50 mg/dL in women)
- High blood pressure (130/80 or above)
- Fatigue disproportionate to sleep quality
- Brain fog and poor concentration (linked to inflammatory cytokines from visceral fat)
If you have three or more of these markers, that cluster is called metabolic syndrome — and visceral fat is its primary driver.
Conclusion
Visceral fat is not a cosmetic problem and it doesn’t respond to cosmetic solutions. It’s a metabolic problem — driven by hormonal shifts, chronic stress, poor sleep, and refined-food diets — and it requires a metabolic response.
Most women see meaningful progress in 6–12 weeks when these elements are applied consistently. Visceral fat is stubborn — but it’s also among the most responsive to lifestyle change of any fat depot in the body. That’s the one piece of genuinely good news here.
Frequently Asked Questions
1. Why am I skinny with visceral fat?
Because visceral fat and body weight are not the same thing. “Normal weight obesity” (sometimes called “skinny fat”) describes individuals with healthy BMI but elevated visceral fat — and it’s more common than people realize. BMI measures total weight relative to height, not fat distribution. A woman can have a BMI of 22 while carrying dangerous levels of visceral fat if her waist circumference exceeds 35 inches. Genetics, low muscle mass, poor diet quality, and chronic stress are primary drivers. (AlignLife)
2. What foods dissolve visceral fat?
No food “dissolves” fat, but several foods demonstrably reduce visceral fat accumulation over time: high-fiber vegetables (especially cruciferous), avocado, fatty fish (omega-3s reduce visceral fat via anti-inflammatory mechanisms), green tea (EGCG has shown modest visceral fat reduction in RCTs), and fermented foods supporting the gut microbiome. The most important dietary moves are eliminating fructose-heavy beverages and ultra-processed foods rather than adding any single “superfood.”
3. How to lose visceral fat in 2 weeks?
You can reduce visceral fat measurably in 2 weeks — primarily through eliminating sugar-sweetened beverages, reducing refined carbohydrates, starting HIIT 3x/week, and improving sleep. However, two weeks is not enough for significant reduction. The most honest answer: 2–4 weeks to see early metabolic improvements (blood sugar, blood pressure), 6–12 weeks for measurable waist reduction with consistent effort. (Healthline)
4. Do healthy people have visceral fat?
Yes. All humans carry some visceral fat — it serves as energy reserve and provides cushioning for organs. The issue is quantity. Visceral fat levels in the “1–9” range on body composition scales, or a waist under 35 inches in women, fall within healthy parameters. Problems arise when levels exceed this threshold and the fat becomes metabolically active at an inflammatory level. (Cleveland Clinic)
5. Can supplements help reduce visceral fat?
Modestly, and only as additions to lifestyle change — not replacements. The best-supported options: fish oil (omega-3s, EPA/DHA), Lactobacillus gasseri probiotics, green tea extract (EGCG), and berberine (which activates AMPK, improving insulin sensitivity). Berberine in particular has shown results comparable to metformin in some studies, though it should be used under supervision. No supplement replaces diet, sleep, and exercise.
6. What is the #1 vegetable to eat more of to reduce visceral fat?
Broccoli — and broadly, cruciferous vegetables. Beyond their fiber content, cruciferous vegetables contain DIM (diindolylmethane) and indole-3-carbinol, which support estrogen metabolism. For perimenopausal and postmenopausal women whose visceral fat accumulation is partly driven by estrogen decline, optimizing estrogen metabolism is relevant — and cruciferous vegetables directly support this pathway.
7. Can you live a long life with visceral fat?
It depends on quantity and trajectory. Chronically elevated visceral fat — particularly above a visceral fat level of 13 on body composition assessments, or a consistent waist circumference above 35 inches — is independently associated with shortened healthspan and increased all-cause mortality risk. However, visceral fat is one of the most responsive fat depots to lifestyle change. Unlike subcutaneous fat, visceral fat shrinks relatively quickly with consistent diet and exercise intervention, giving it a more reversible risk profile.
Medical disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider for personalized guidance, particularly regarding hormonal health and metabolic conditions.
← Back to all posts