How To Get Rid Of Pcos Belly
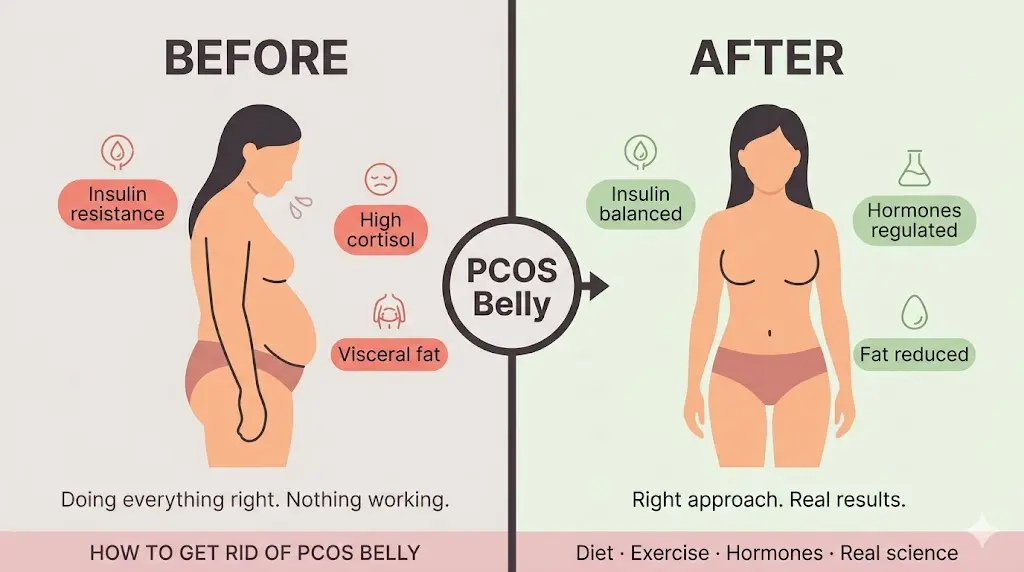
How to Get Rid of PCOS Belly (What Actually Works, From Someone Who Gets It)
KEY TAKEAWAYS
- PCOS belly is driven by insulin resistance and high cortisol — not just calories. Treating the root cause is what actually moves the needle.
- Strength training beats cardio for PCOS fat loss. Building muscle is the single most effective way to improve insulin sensitivity and shrink abdominal fat.
- Diet timing and food quality matter more than restriction. A low-glycemic, anti-inflammatory approach — paired with real sleep and stress management — is the combination that works.
There’s a specific kind of exhausting that comes with PCOS belly. You eat well. You work out. You do everything “right.” And yet there it is — that stubborn, rounded belly that refuses to budge no matter what you try.
You’ve probably Googled every variation of this topic at 11pm more than once. So have I.
One Reddit user put it so perfectly it broke my heart a little: “I’m at a point where I’m considered skinny, and everyone thinks so because I’m always wearing baggy clothing. But I have a huge, bloated belly, and everyone who sees it is always shocked or thinks I’m pregnant. I’ve been seeing a gym trainer for over a year, and she herself is frustrated.”
If that hit close to home — you’re not alone, and you’re not broken. Let’s actually talk about what’s happening in your body, and more importantly, what you can do about it.
First, Let’s Talk Numbers
PCOS (Polycystic Ovary Syndrome) affects 8–13% of women of reproductive age worldwide, according to the World Health Organization. But here’s the part that really gets me: up to 70% of affected women go undiagnosed. That means millions of us are out here fighting symptoms we can’t even name.
If you know you have PCOS, you’re already one step ahead. And the fact that you’re reading this means you’re not willing to just live with it — good. Because the research shows that with the right approach, symptoms — including that stubborn belly — are very much manageable.
What Is PCOS Belly, Exactly?
PCOS belly, a type of belly fat, isn’t just regular bloating or garden-variety weight gain. It’s a very specific pattern of abdominal fat accumulation driven primarily by insulin resistance.
Here’s what’s actually happening: when your cells don’t respond properly to insulin, your pancreas pumps out more of it to compensate. High insulin levels signal your body to store fat — and they’re especially good at directing that fat to your midsection.
Add elevated androgens (male hormones like testosterone that are elevated in many women with PCOS) and chronic low-grade inflammation to the mix, and you’ve got a recipe for stubborn visceral fat that doesn’t respond to typical diet-and-exercise advice.
A 2019 study published in Obesity Reviews confirmed that women with PCOS carry significantly more visceral adipose tissue (the deep belly fat surrounding organs) compared to women without PCOS, even at the same BMI.
PCOS Belly Shape vs. Normal Belly — What’s the Difference?
Visually, PCOS belly tends to sit differently than typical weight gain. Most people store fat in a more even, diffuse pattern. PCOS belly tends to be:
- Round and protruding, often described as looking pregnant or like a “pot belly”
- Firm to the touch, not just soft and squishy — because it’s visceral fat deeper in the abdominal cavity, not subcutaneous fat just under the skin
- Concentrated in the upper-to-mid abdomen, rather than lower belly or hips
- Disproportionate to the rest of the body — this is the tell-tale sign
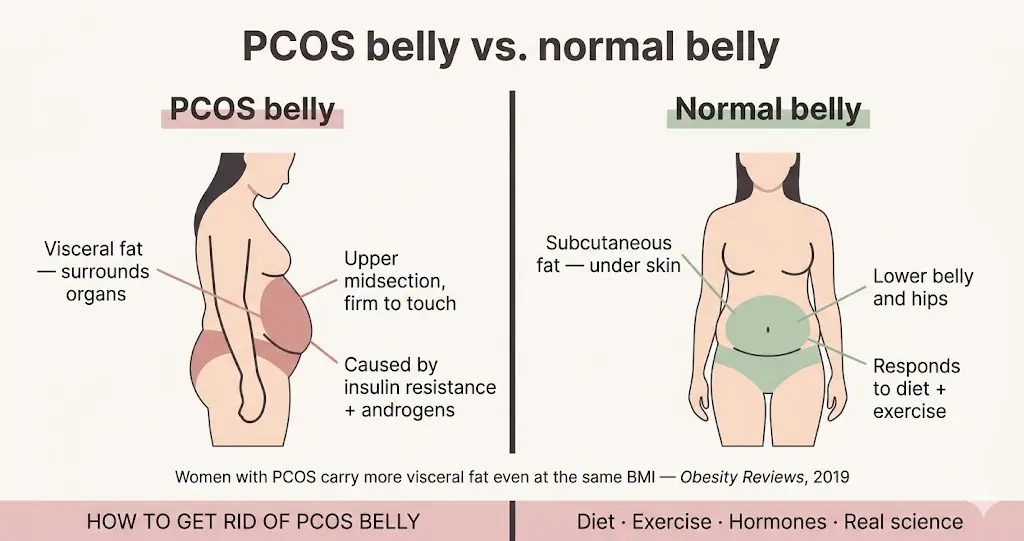
The key distinction is location. Normal belly fat accumulates subcutaneously. PCOS belly is largely visceral — it’s inside, wrapping around your organs, which is why it’s both more visible as a protrusion and more metabolically active.
PCOS Belly on a Skinny Person
This is the part people don’t talk about enough, and it needs to change. PCOS belly absolutely shows up on women who are otherwise thin or at a “healthy” weight. It’s called lean PCOS, and it’s more common than most people realize.
Research from the Journal of Clinical Endocrinology & Metabolism shows that lean women with PCOS still present with metabolic abnormalities including insulin resistance, elevated androgens, and the same pattern of centralized fat distribution — even when their total body weight appears normal. If your waist-to-hip ratio is high despite a low BMI, PCOS is a very plausible explanation.
So if a gym trainer is frustrated that your belly won’t shift despite clean eating and consistent training — it’s not your discipline that’s the problem. It’s the underlying hormonal environment.
PCOS Belly Symptoms
Beyond just the visible belly, PCOS belly often comes with a cluster of symptoms that confirm what’s happening hormonally.

The Cleveland Clinic notes that abdominal obesity in PCOS is strongly correlated with increased risk of metabolic syndrome, type 2 diabetes, and cardiovascular disease — which is why addressing it matters far beyond aesthetics.
PCOS Belly Diet — What to Eat, What to Skip, and When
Let me be direct with you: no single “magic” food fixes PCOS belly. But the pattern of eating absolutely matters, and the research is fairly clear on what helps.
What Is the Best Diet for PCOS and Thyroid?
Many women with PCOS also have thyroid dysfunction (hypothyroidism is more common in PCOS). The overlap means your diet needs to work for both — and fortunately, the approach is largely the same:
- Low-glycemic, high-fiber foods to manage insulin and support thyroid hormone conversion
- Anti-inflammatory foods — think omega-3s, colorful vegetables, olive oil — which support both PCOS and thyroid health
- Adequate iodine and selenium (from foods like eggs, seafood, Brazil nuts) for thyroid function
- Limiting goitrogens in excess (raw cruciferous veg like raw kale in large amounts) if thyroid is already compromised — though cooked versions are fine
A 2021 systematic review in Nutrients found that low-GI diets significantly improved insulin sensitivity, hormonal profiles, and body composition in women with PCOS.
##PCOS Diet: What to Eat Vs. What to Skip?
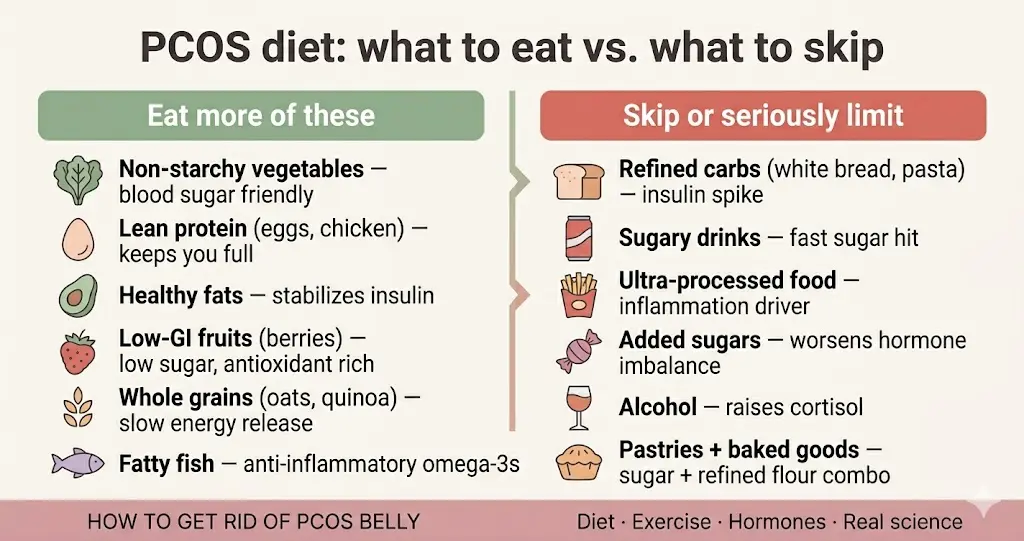

How Many Times Should You Eat a Day?
For PCOS, the goal is blood sugar stability. Here’s what actually works:
- 3 balanced meals a day with 1–2 optional snacks if genuinely hungry
- Never skip breakfast — research shows eating a larger breakfast and smaller dinner improves insulin and testosterone levels in women with PCOS
- Aim for a 12-hour eating window if possible — e.g., 8am to 8pm — to give your insulin time to reset
- Don’t graze constantly — every time you eat, you spike insulin, even mildly
Best Fruits for PCOS
Not all fruit is created equal for PCOS. Go for low-GI options like berries, cherries, apples, pears, and citrus — fruits that release sugar slowly and won’t spike your insulin.

Best Breakfast, Dinner, and Snacks for PCOS
Focus on protein-forward breakfasts (eggs, Greek yogurt, nuts), balanced dinners with lean protein and non-starchy vegetables, and snacks like hummus with veggies, a small handful of nuts, or a boiled egg.

PCOS Belly Fat Reduction Exercises — What Actually Moves the Needle
Here’s where most advice gets it backward. We’re told to do more cardio to lose fat. But for PCOS, endless cardio can actually backfire — it raises cortisol, which raises insulin, which tells your body to hold onto belly fat. Not the goal.
The research is pretty clear: strength training is the most effective exercise for PCOS-related fat loss. A 2020 meta-analysis in the Journal of Functional Morphology and Kinesiology found that resistance training improved insulin sensitivity, reduced testosterone levels, and improved body composition in women with PCOS — more effectively than cardio alone.
What to Do
Strength training 2–3 times per week: compound movements like squats, deadlifts, lunges, push-ups, and rows are your best friends. Building muscle increases glucose uptake independent of insulin. Growwithjo is the one I rely on — she makes the workouts enjoyable and exciting.
Walking — don’t underestimate it: a 20–30 minute walk after meals is one of the most effective ways to blunt post-meal blood sugar spikes. It’s low cortisol, sustainable, and surprisingly effective.
Yoga and Pilates: both reduce cortisol and support hormonal balance. A 2022 study in the Journal of Education and Health Promotion found yoga specifically improved PCOS symptoms including hormonal markers and psychological wellbeing. Move With Nicole is my favourite yoga instructor.
HIIT in moderation: short, intense intervals (like 20 minutes, twice a week max) can improve insulin sensitivity, but overdoing it raises cortisol. Keep it brief. Growingannanas is your buddy for this.
What to Avoid
- Long daily cardio sessions (running for 60+ minutes daily raises cortisol significantly)
- Overtraining — rest days are metabolically necessary, not a luxury
- Exercising fasted if it stresses you out — some women do well with fasted workouts, others don’t. If you feel anxious or dizzy, eat something first.
The general guideline from the American College of Sports Medicine is 150 minutes of moderate activity per week — but for PCOS, the quality and type of exercise matters more than hitting a number.
Conclusion
PCOS belly is real, it’s specific, and it responds to a very specific set of interventions. This isn’t about eating less and moving more — that approach misses the entire hormonal picture. What actually works is:
- A low-glycemic, anti-inflammatory diet that keeps insulin stable
- Strength training as your primary exercise mode
- Stress management — not optional, actually metabolic
- Sleep of 7–9 hours — poor sleep increases cortisol and insulin resistance within days
- Patience — this is a hormonal condition, and hormonal shifts take weeks to months, not days
I want to be honest with you: some women also need medical support. Metformin, inositol supplementation, or hormonal therapy can all be part of the picture, and there’s no shame in that. If you’ve been doing everything “right” for months and nothing is shifting, please talk to an endocrinologist, not just a general practitioner. You deserve a doctor who takes this seriously.
You are not failing. You are fighting a hormonal condition with incomplete information. Now you have a little more. Go use it.
Frequently Asked Questions
What happens to the body with PCOS?
PCOS disrupts the normal hormonal cycle that governs ovulation. The ovaries produce excess androgens (male hormones), which interferes with egg development and release. This creates a cascading effect: irregular or absent periods, cyst formation on the ovaries, insulin resistance, inflammation, and a higher risk of metabolic conditions like type 2 diabetes, cardiovascular disease, and non-alcoholic fatty liver disease. Symptoms vary enormously between women — some have all of them, some have only a few. The condition is also closely linked to thyroid dysfunction and adrenal irregularities.
What is the 30 30 30 rule for PCOS?
The 30-30-30 rule has gained traction on social media and was popularized by health educator Gary Brecka. It involves: 30 grams of protein within 30 minutes of waking up, followed by 30 minutes of low-intensity movement (like walking). The idea is to stabilize blood sugar and cortisol from the moment you start your day. While there’s no PCOS-specific clinical trial on this exact protocol, it aligns well with established research on the benefits of high-protein breakfasts for insulin management and morning exercise for blood sugar regulation. For PCOS, it’s worth trying — it’s low-risk and biologically sound.
What is the first stage of PCOS?
PCOS doesn’t have formally staged progressions the way some conditions do, but early signs often include irregular periods (or periods that were regular and become irregular), mild hormonal symptoms like acne or excess hair growth, and subtle metabolic changes detectable on bloodwork (elevated androgens, slightly elevated insulin). Many women first notice something is off in their teens or early twenties. Early intervention — especially lifestyle-based — is genuinely impactful and can prevent the condition from worsening.
Are you 100% infertile with PCOS?
No — absolutely not. PCOS is one of the most common causes of infertility, but “common cause” does not mean “guaranteed infertility.” Many women with PCOS conceive naturally, and many more conceive with relatively minimal intervention such as lifestyle changes, ovulation induction medications (like letrozole or clomiphene), or IVF. A 2020 review in Frontiers in Endocrinology notes that with appropriate management, the majority of women with PCOS who want to conceive are able to do so. Please don’t let fear about fertility stop you from getting a diagnosis — knowing is always better than not knowing.
← Back to all posts